One of the wonderful things about dry eye disease (DED) is that technicians can utilize both their physical skills and their accumulated knowledge to produce a high quality patient work-up, ultimately leading to better patient care.
In particular, in-office diagnostic testing has become a linchpin in many practices that emphasize DED care. Over the last several years, it has become increasingly obvious that any practice that offers cataract and refractive surgery must also be proficient in the diagnosis and treatment of DED as well. Whether working through a standardized protocol or empowered to do testing when a patient’s history suggests a possible DED diagnosis, information gathered by the eye-care technician through diagnostic tests will ultimately clinch the diagnosis and inform the treatment plan.
It stands to reason that the more specific we can be when it comes to the type of DED, the presence or absence of inflammation, and any associated structural changes present in the lacrimal functional unit (lacrimal gland/goblet cells/meibomian glands), the more precisely we can target our treatment. Here, I will review the DED tests at our collective disposal.
Tear production and volume
We begin with one of the oldest tests in all of eye care: the Schirmer test. Once upon a time, all DED was thought to be caused by decreased tear production and volume, which could be measured via Schirmer testing.
The test involves placing a standardized strip of filter paper in the inferior cul-de-sac just under the lower lid. Anesthetizing the eye is felt to give a result that indicates the baseline volume of tear production, whereas doing the test without anesthesia will give an indication of the maximum ability to produce tears. Some practices will also instill a dye such as fluorescein to make measuring easier. In either test, a strip that has less than 10 mm of moistening over 5 minutes is abnormal.
Tear characteristics
Measuring the characteristics of the tears themselves can be done in many ways. The oldest of these is lactoferrin levels, a test that has been on the market since the 1990s. Low lactoferrin levels measured with an instrument such as the Tear Scan 270 Micro Assay (Advance Tear Diagnostic) indicates DED. For mostly economic reasons, lactoferrin testing has not caught on, although experts such as Joe Tauber, MD, have been seeking to change this.
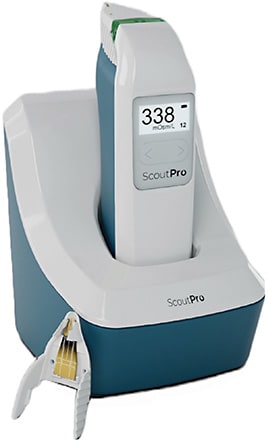
Tear osmolarity (TO) testing has been around almost as long as lactoferrin. Here, a single company has led the charge from the beginning. TearLab recently re-branded as Trukera Medical in preparation for an expansion into new diagnostic tests and treatments on the ocular surface. Trukera’s first product is a significant upgrade to their classic TO instrument. The ScoutPro Osmolarity System is a self-contained handheld instrument that reads TO on the instrument itself; you no longer need to return the handheld to its base to receive the result. Each unit has a rechargeable battery. In our trials, the battery lasted longer than a full office day.
Elevated TO (above 208 mOsm/L) is always abnormal and indicates a loss of homeostasis on the ocular surface. Asymmetry greater than 8 mOsm/L between the eyes indicates the same, regardless of the absolute level. Trukera continues to manufacture the only FDA-approved instrument to measure TO.
Inflammation
Determining whether inflammation is present on the ocular surface can drive treatment decisions, particularly the use of topical steroids. Testing using InflammaDry (Quidel) gives us a qualitative (positive or negative) result regarding the presence of MMP-9, a marker of inflammation.
The qualitative nature of the test means that it is difficult to tell if intervention has made a meaningful change in surface inflammation. Nonetheless, many doctors continue to find value here, especially in the initial exam.
Meibography
The newest, and perhaps most impactful among the standard DED diagnostic tests is meibography. Imaging the meibomian glands allows the doctor and patient to visualize what is often the direct cause of DED symptoms.
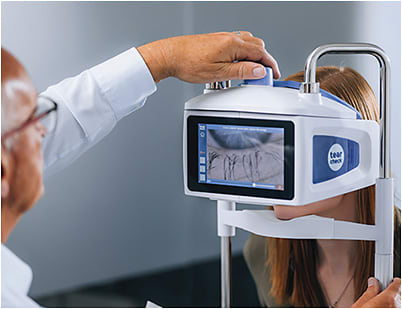
Technicians play a particularly important role when they perform meibography, explaining the results in real time to the patient. LipiView and its smaller sibling LipiScan (J&J Vision) were the first instruments to enjoy widespread use in both ophthalmology and optometry. Newer instruments such as MeiBox (Box Medical Solutions) and TearCheck (E-SWIN USA) have entered the market and provided low-cost options to practices.
The consensus among DED doctors is that evaporative DED is by far the more common type seen in our practices. Meibography is the gateway to our most modern treatments; thermal, thermal with evacuation, and light-based therapies are all strongly supported when meibography shows abnormal gland function and/or gland destruction.
Corneal topography
Lastly, corneal topography has emerged in the diagnosis of DED. Surgical patients expect near perfect refractive outcomes from pretty much all of the anterior segment surgeries we perform. Along with laser refractive surgeries and refractive cataract procedures with advanced technology implants to correct astigmatism and presbyopia, patients now have the same high expectations with standard monofocal IOLs as well.
Corneal topography used in the pre-op evaluation for cataract and refractive laser patients can be the tip-off that DED needs to be addressed before surgery. The technician doing a pre-op work-up is often the first person to put up a DED red flag after seeing an irregular topography.
Conclusion
Diagnostic tests performed by technicians are a part of the foundation of DED care. Sadly, our testing armamentarium is largely unchanged over the last 5 years. However, more experience with the tests we do have has increased the value of their input. While performing these tests, technicians may be the first members of the team to suspect DED. Making and then refining the DED diagnosis inevitably leads to better outcomes for patients. OP









